Problem
A large women’s health organization—with an in‑house lab and Level‑III neonatology unit—was losing Medicaid revenue fast. Offshore billing restrictions left large portions of Medicaid AR untouched, while overwhelmed internal teams struggled with Medicaid‑specific rules, maternity protocols, and eligibility complexity. As denials climbed, the group wrote off $1.3M in Medicaid bad debt per year in both 2023 and 2024, with early 2025 trending towards the same costly outcome.
Solution
To stop the financial decline, the practice deployed Connective Health’s Medicaid RCM Solution. We deployed a targeted remediation plan designed to recover at‑risk revenue and fix root‑cause workflow breakdowns. This included a Medicaid AR Mitigation Project to work aging claims, strengthened pre‑claim edits to prevent documentation and coding errors, a Medicaid billing catalogue to empower staff, and a full overhaul of eligibility and authorization processes across all sites
The results were immediate and transformative. Within 10 months, the organization achieved the following:
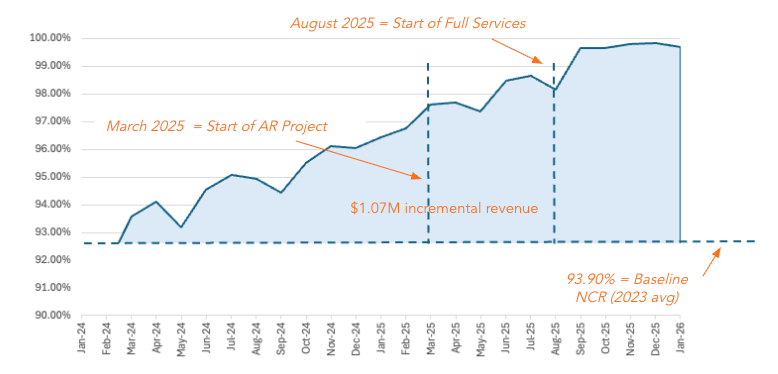
- $1.07M in incremental Medicaid collections
- Net Collections Rate (NCR) to over 99.0% on a consistent basis
- 3.33x return on investment (ROI)
- DAR reduction of 2.7 days
- Consistent front‑end eligibility accuracy
- Higher‑quality coding and documentation compliance to payers